Anticonvulsants, also known as antiepileptic or antiseizure drugs, are a class of pharmacological agents used in the prevention and control of seizures, primarily in patients suffering from Epilepsy. These drugs do not cure epilepsy but suppress abnormal neuronal excitability and prevent the recurrence of seizures.
Seizures arise due to excessive, synchronous electrical discharge in neurons of the brain, which may result from imbalances between excitatory neurotransmitters (e.g., glutamate) and inhibitory neurotransmitters (e.g., GABA).
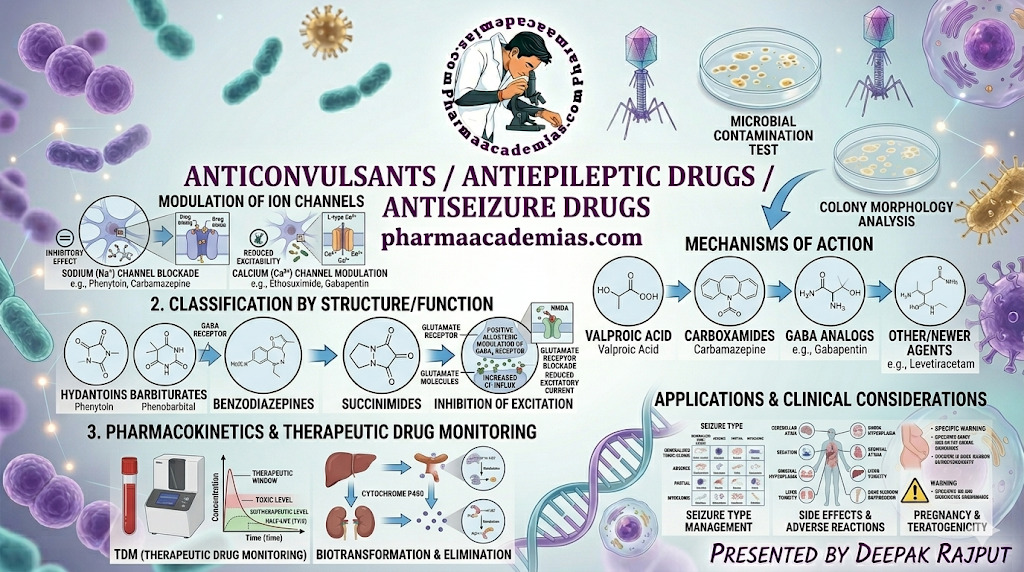
Classification of Anticonvulsants Drugs
Antiepileptic drugs can be classified based on mechanism of action and clinical use.
1. Sodium Channel Blockers
Sodium channel blockers constitute one of the most important classes of AEDs. These drugs act by stabilizing the inactive state of voltage-gated sodium (Na⁺) channels, thereby preventing repetitive and sustained neuronal firing. By prolonging the refractory period of neurons, they effectively limit the propagation of abnormal electrical signals responsible for seizures.
Examples include:
- Phenytoin
- Carbamazepine
- Lamotrigine
They are particularly effective in partial and generalized tonic-clonic seizures.
2. Calcium Channel Modulators
This class primarily targets T-type calcium (Ca²⁺) channels, which are predominantly found in thalamic neurons and play a crucial role in the generation of rhythmic cortical discharges seen in absence seizures.
Example:
- Ethosuximide
It is the drug of choice for absence seizures.
3. GABAergic Drugs (Enhancers of Inhibition)
Gamma-aminobutyric acid (GABA) is the principal inhibitory neurotransmitter in the central nervous system. Drugs in this category enhance GABAergic transmission, thereby increasing neuronal inhibition and reducing seizure activity.
Examples include:
- Diazepam
- Phenobarbital
- Valproic acid
They increase GABA levels by:
- Enhancing receptor activity
- Inhibiting GABA degradation
- Increasing GABA synthesis
4. Glutamate Inhibitors
Glutamate is the primary excitatory neurotransmitter in the brain. Excessive glutamatergic activity contributes significantly to seizure generation. Drugs in this class work by inhibiting glutamate-mediated excitatory neurotransmission.
Examples:
- Topiramate
- Felbamate
5. SV2A Protein Modulators
This is a relatively newer class of AEDs that target synaptic vesicle protein 2A (SV2A), a protein involved in neurotransmitter release at synaptic terminals.
Example:
- Levetiracetam
They are widely used due to better safety profile and minimal drug interactions.
6. Mixed Mechanism Drugs
Some AEDs exhibit multiple mechanisms of action, making them highly effective across a broad range of seizure types. These drugs target different pathways simultaneously, enhancing their therapeutic efficacy.
Example:
- Valproic acid (Blocks Na⁺ channels, increases GABA, and inhibits Ca²⁺ channels)
Mechanism of Action of Anticonvulsants
The pharmacological action of antiepileptic drugs revolves around restoring the balance between neuronal excitation and inhibition.
One major mechanism is the blockade of voltage-gated sodium channels, which prevents repetitive firing of neurons. Drugs like phenytoin and carbamazepine prolong the inactivated state of sodium channels, thereby stabilizing neuronal membranes.
Another important mechanism involves enhancement of GABAergic transmission, which increases inhibitory tone in the central nervous system. Benzodiazepines like diazepam enhance the frequency of chloride channel opening, whereas barbiturates like phenobarbital prolong its duration.
Certain drugs reduce calcium influx through T-type calcium channels, which is particularly relevant in absence seizures where thalamocortical circuits are involved.
Additionally, newer drugs like levetiracetam modulate synaptic vesicle proteins, reducing neurotransmitter release and neuronal excitability.
Clinical Uses of Anticonvulsants Drugs
Antiepileptic drugs are used in a variety of seizure disorders and other neurological conditions.
1. Epilepsy Management
- Generalized tonic-clonic seizures
- Absence seizures
- Partial (focal) seizures
- Myoclonic seizures
2. Status Epilepticus
A life-threatening condition requiring immediate treatment with:
- Diazepam
- Lorazepam
3. Other Therapeutic Uses
Many AEDs are used beyond epilepsy:
- Neuropathic pain (e.g., carbamazepine in trigeminal neuralgia)
- Bipolar disorder (valproic acid, lamotrigine)
- Migraine prophylaxis (topiramate, valproate)
Adverse Effects of Antiepileptic Drugs
The adverse effects vary depending on the drug but commonly include:
Central nervous system effects such as sedation, dizziness, ataxia, and cognitive impairment are frequently observed. Long-term use may lead to tolerance and dependence, particularly with benzodiazepines.
Some drugs produce idiosyncratic reactions, such as:
- Skin rashes (Stevens-Johnson syndrome with lamotrigine)
- Hepatotoxicity (valproic acid)
- Gingival hyperplasia (phenytoin)
Teratogenicity is a major concern, especially with valproic acid, which can cause neural tube defects.
Drug Interactions
Many antiepileptic drugs are enzyme inducers or inhibitors, affecting hepatic cytochrome P450 enzymes.
- Phenytoin and carbamazepine are strong enzyme inducers
- Valproic acid is an enzyme inhibitor
This leads to significant interactions with:
- Oral contraceptives
- Anticoagulants
- Other CNS drugs
Recent Advances in Antiepileptic Therapy
Modern therapy focuses on drugs with:
- Better safety profile
- Minimal drug interactions
- Broad-spectrum activity
Newer agents such as levetiracetam and lamotrigine have gained popularity due to improved tolerability and efficacy. Research is also ongoing into gene therapy, neurostimulation (vagus nerve stimulation), and personalized medicine.
Conclusion
Anticonvulsants or antiepileptic drugs are a cornerstone in the management of epilepsy and related neurological disorders. Their mechanism involves modulation of ion channels, enhancement of inhibitory neurotransmission, and suppression of excitatory pathways.







3 Comments