Syphilis
Syphilis is a chronic systemic infectious disease caused by the spirochete bacterium Treponema pallidum subspecies pallidum. It is primarily transmitted through sexual contact, but can also be congenitally acquired. Known for its multistage progression, if left untreated, syphilis may lead to serious cardiovascular, neurological, and dermatological complications over time.
Once on the decline due to effective antibiotic use, the global re-emergence of syphilis in the 21st century has sparked new interest in its epidemiological surveillance, public health strategies, and advanced therapeutic approaches.
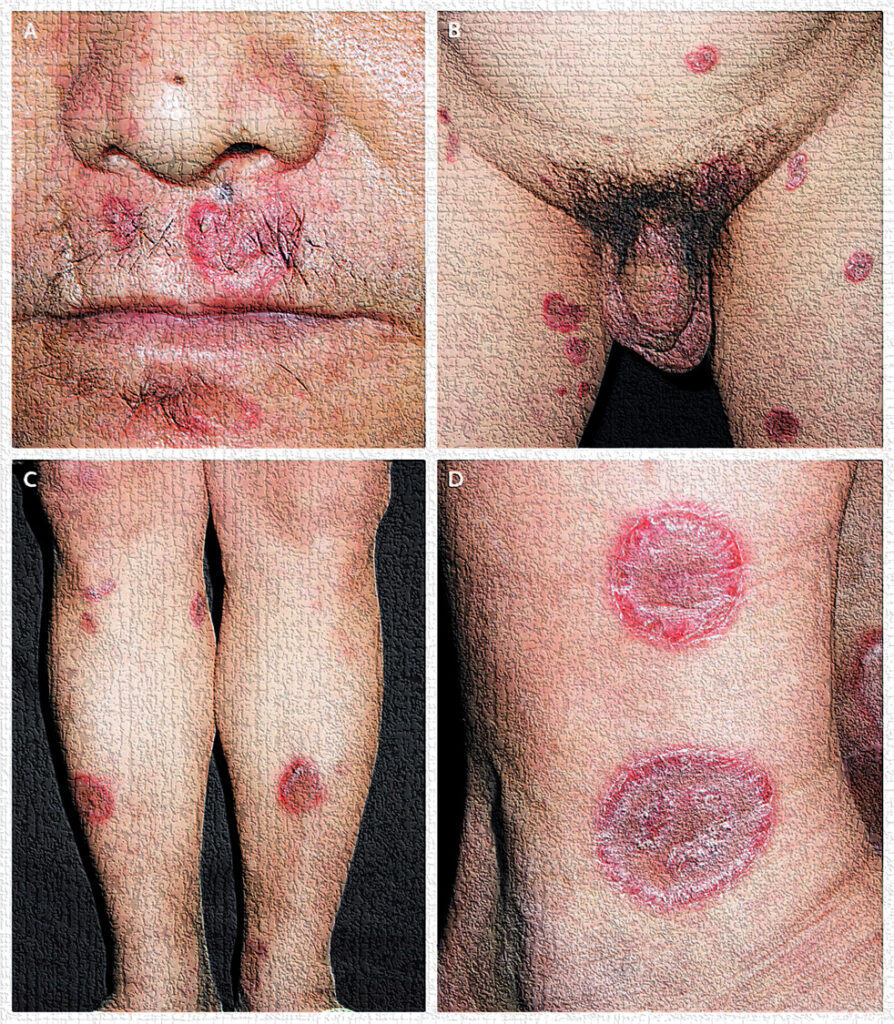
2. Definition
Syphilis is a sexually transmitted infection (STI) that progresses through distinct stages: primary, secondary, latent, and tertiary. Each stage is characterized by unique clinical features and potential systemic involvement. If untreated, syphilis can persist for decades and lead to serious health consequences, including neurosyphilis, cardiovascular syphilis, and congenital syphilis in neonates.
3. Epidemiology of Syphilis
3.1 Global Burden
- As per the World Health Organization (WHO, 2023), an estimated 7.1 million new syphilis infections occur each year.
- It accounts for approximately 6% of all curable STIs globally.
- Syphilis also significantly contributes to adverse pregnancy outcomes like stillbirth, neonatal death, and congenital infection.
3.2 Trends and High-Risk Groups
- Resurgence has been reported in men who have sex with men (MSM), particularly those co-infected with HIV.
- Prevalence is higher among sex workers, migrant populations, and people with multiple sexual partners.
- Urban and socioeconomically disadvantaged communities remain disproportionately affected.
3.3 India Scenario
- According to the National AIDS Control Organization (NACO), syphilis accounts for a substantial portion of STI clinic visits.
- Congenital syphilis continues to be a concern due to poor antenatal screening in some regions.
4. Etiology
Syphilis is caused by Treponema pallidum subsp. pallidum, a slender, helically coiled spirochete bacterium with the following characteristics:
- Gram-negative-like structure, but does not stain well.
- Cannot be cultured on artificial media.
- Highly motile, allowing it to disseminate throughout the body rapidly.
- Sensitive to heat, drying, and disinfectants.
Other non-venereal Treponema species cause similar diseases:
- T. pertenue → Yaws
- T. endemicum → Bejel
- T. carateum → Pinta
5. Mode of Transmission
Syphilis is highly contagious during its primary and secondary stages. It spreads via:
- Sexual contact – through direct contact with syphilitic sores (chancres) during vaginal, anal, or oral sex.
- Congenital transmission – across the placenta during pregnancy.
- Blood transfusion – though rare, as blood is now screened.
- Contact with infectious lesions – via non-sexual close contact (rare).
Note: Transmission is not possible via toilet seats, swimming pools, or casual physical contact.
Pathophysiology of Syphilis
Step 1: Entry of Bacteria
Syphilis is caused by Treponema pallidum, a thin spiral-shaped bacterium (spirochete). It usually enters the body through sexual contact by small cuts or abrasions in the skin or mucous membranes of the genital area, mouth, or rectum.
Step 2: Local Infection (Primary Stage)
After entry, the bacteria multiply at the site of infection. This causes a small, painless sore called a chancre. The sore appears about 2–3 weeks after exposure and is highly infectious. At this stage, the bacteria also begin to spread into nearby lymph nodes.
Step 3: Spread Through the Blood (Secondary Stage)
The spirochetes then enter the bloodstream and spread throughout the body. This causes a widespread immune reaction, leading to rash, fever, swollen lymph nodes, sore throat, and muscle aches. The rash often appears on the palms and soles. Because the bacteria circulate everywhere, this stage is very infectious.
Step 4: Latent Stage
After the secondary stage, the infection may become latent (hidden). During this time, the bacteria remain in the body without causing noticeable symptoms. The latent stage can last for years. Some patients remain symptom-free, while in others the disease progresses silently.
Step 5: Tertiary Stage (Late Syphilis)
If untreated, syphilis can progress to the tertiary stage years later. At this stage, the bacteria cause severe tissue and organ damage. Typical effects include gummas (destructive granulomas in skin and bones), damage to the heart and blood vessels (aortic aneurysm), and nervous system involvement (neurosyphilis). These changes can be disabling or fatal.
6. Pathogenesis
- Inoculation: The spirochetes penetrate microabrasions on mucosal or epithelial surfaces.
- Local replication: Multiplication occurs at the entry site forming a chancre.
- Lymphatic and hematogenous spread: Rapid dissemination to various organs and tissues.
- Immune evasion: T. pallidum lacks classic pathogen-associated molecular patterns (PAMPs), helping it evade host immunity.
- Chronic inflammation: Leads to long-term damage in organs during tertiary stages.
7. Types and Stages of Syphilis
Syphilis progresses through distinct clinical stages if untreated:
7.1 Primary Syphilis
- Incubation: 10–90 days post-exposure.
- Characterized by a painless ulcer (chancre) at the site of entry (genitals, anus, lips).
- Local lymphadenopathy.
- Chancre heals spontaneously in 3–6 weeks even without treatment.
7.2 Secondary Syphilis
- Occurs weeks to months after the chancre heals.
- Systemic spread of spirochetes.
- Symptoms include:
- Maculopapular rash, including on palms and soles.
- Mucous patches, condyloma lata (moist, wart-like lesions).
- Fever, malaise, sore throat.
- Patchy alopecia.
- Hepatitis, meningitis (rare).
- Highly infectious phase.
7.3 Latent Syphilis
- Early latent: Within 1 year of infection; potentially infectious.
- Late latent: After 1 year; less infectious.
- Asymptomatic, but serologically positive.
- May last for years or decades.
7.4 Tertiary (Late) Syphilis
- Appears 10–30 years after infection.
- Less common in the antibiotic era.
- Characterized by:
- Gummatous syphilis – granulomatous lesions in skin, liver, bones.
- Cardiovascular syphilis – aortitis, aortic aneurysm.
- Neurosyphilis – tabes dorsalis, general paresis, meningovascular involvement.
7.5 Congenital Syphilis
- Transmitted from mother to fetus during pregnancy.
- Early signs (within 2 years): nasal discharge, rash, hepatosplenomegaly.
- Late signs: Hutchinson’s triad (interstitial keratitis, notched incisors, deafness), saddle nose, saber shins.
8. Clinical Manifestations
| Stage | Features |
| Primary | Chancre (painless ulcer), inguinal lymphadenopathy |
| Secondary | Rash, condyloma lata, fever, sore throat, patchy hair loss |
| Latent | No symptoms, only positive serology |
| Tertiary | Gummas, aortic aneurysm, neurosyphilis symptoms (ataxia, dementia) |
| Congenital | Snuffles, bone deformities, developmental delay, Hutchinson’s triad |
9. Diagnosis
9.1 Direct Detection
- Dark field microscopy: Visualizes T. pallidum from lesion exudates.
- Direct fluorescent antibody test (DFA-TP).
9.2 Serologic Tests
Non-treponemal Tests (Screening)
- VDRL (Venereal Disease Research Laboratory)
- RPR (Rapid Plasma Reagin)
- Detect antibodies against cardiolipin (not specific to T. pallidum).
- Titers help monitor treatment response.
Treponemal Tests (Confirmatory)
- FTA-ABS (Fluorescent Treponemal Antibody-Absorption)
- TPHA (Treponema pallidum Hemagglutination Assay)
- More specific; remain positive for life.
9.3 CSF Examination
- For suspected neurosyphilis: VDRL, cell count, protein in cerebrospinal fluid.
10. Treatment of Syphilis
10.1 First-Line Treatment
Early Syphilis (Primary, Secondary, Early Latent)
- Benzathine Penicillin G 2.4 million units IM single dose
Late Latent or Tertiary (without neurosyphilis)
- Benzathine Penicillin G 2.4 million units IM weekly × 3 doses
Neurosyphilis
- Aqueous crystalline Penicillin G 18–24 million units/day IV, divided every 4 hours × 10–14 days
10.2 Alternatives for Penicillin-Allergic Patients
- Doxycycline 100 mg orally BID × 14 days (early) or × 28 days (late).
- Tetracycline 500 mg orally QID.
- For neurosyphilis, desensitization followed by penicillin is preferred.
10.3 Treatment in Pregnancy
- Penicillin is the only recommended treatment.
- Penicillin allergy → desensitization and then penicillin therapy.
10.4 Follow-Up
- Serologic titers (e.g., VDRL) should be monitored at 6, 12, and 24 months.
- Four-fold drop in non-treponemal titers indicates successful treatment.
11. Prevention and Control
- Condom use and safe sex practices.
- Routine STI screening for high-risk individuals.
- Partner notification and treatment.
- Antenatal screening to prevent congenital syphilis.
- Public awareness campaigns and sex education.
- No vaccine is currently available.
12. Complications if Untreated
- Aortic aneurysm, aortitis
- CNS damage: Tabes dorsalis, general paresis
- Blindness, deafness
- Bone deformities
- Vertical transmission leading to fetal loss or birth defects
Conclusion
Syphilis, though an ancient disease, continues to challenge public health systems globally. With its complex clinical course, varied manifestations, and potential for severe late complications, early diagnosis and effective treatment remain paramount. Penicillin continues to be the cornerstone of therapy, and timely antenatal screening is vital in preventing congenital syphilis. In an era where STIs are resurging, robust awareness programs, sexual health education, and epidemiological monitoring are crucial for controlling syphilis and its consequences.